Welcome to the CODA study website!
The COVID and Diabetes Assessment study’s goal is to gain a deeper understanding of what happens in the first one to two years after a diagnosis of diabetes. The study will examine the possible impact of COVID-19 and other factors on early diabetes. The study will recruit patients recently diagnosed with diabetes and follow them closely to see how various factors – including COVID-19 infections, diabetes medications, diet, and exercise – impact their diabetes. Some studies have suggested that these factors may impact both Type 1 diabetes (T1D) or Type 2 diabetes (T2D) development and progression. This study will help us to better understand these issues.
Who can participate in this study?
The Study will enroll about 1,000 participants. All participants must be age 11 or older, and have been diagnosed with diabetes in the last six months.
- Diagnosed with Type 1 or Type 2 diabetes in the last 6 months
- Age 11 years or older
How will this study work?
Individuals who agree to participate in the study will be surveyed by phone, online or in person and will provide regular blood samples. A subset of participants will be asked to participate in additional tests that measure glucose tolerance, biomarkers and vascular function testing. Participants will be followed for 1 ½ years (18 months). The study will also leverage longitudinal electronic health record data.


The CODA study will explore:
- How various factors - such as COVID-19 infections, diabetes medications, diet, and exercise – relate to blood sugar control, inflammation, and insulin resistance in patients with T2D
- How these various factors relate to blood sugar control, inflammation, and beta cell function in patients who develop T1D
- How these various factors relate to vascular function, inflammation, and tendency to form blood clots in patients with diabetes
- The role of genetic, social, and environmental factors on inflammation and metabolic function
- The impact of COVID-19 and its treatments on the development of diabetes and on diabetes-related outcomes over the course of time
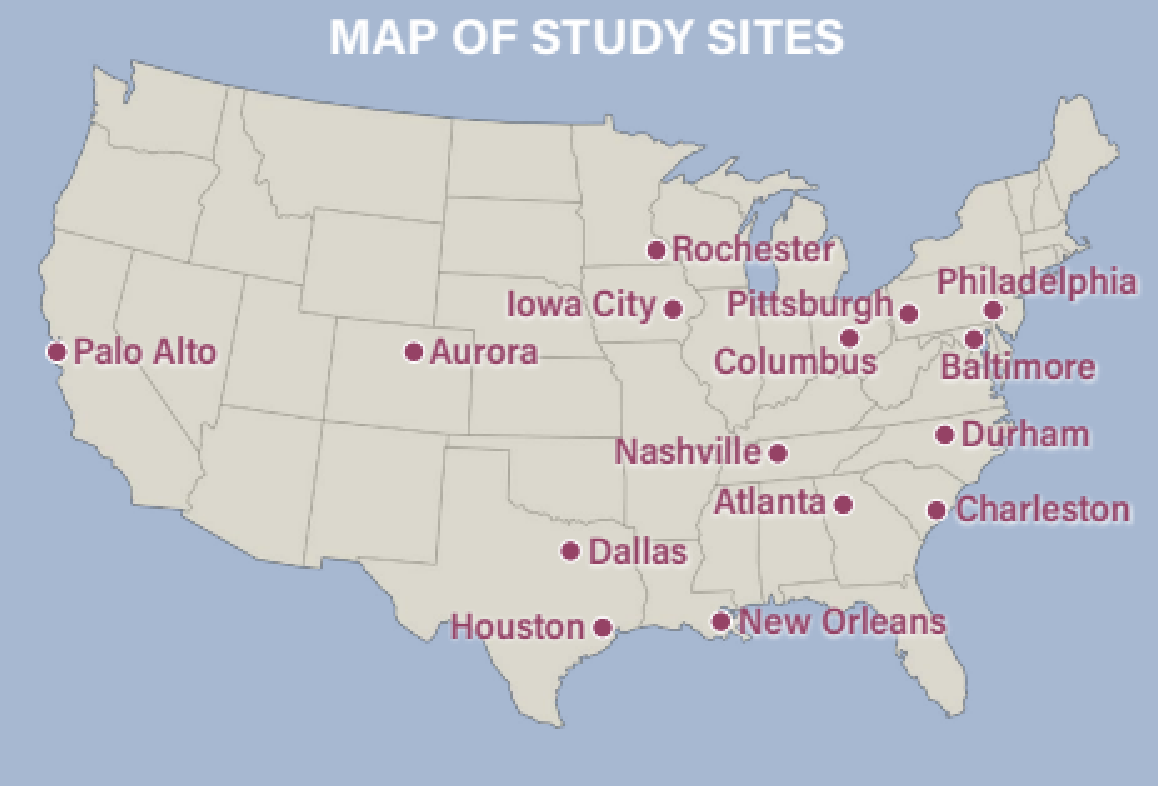
Where will this study take place?
This map shows the locations of all the CODA study sites. City names in the adjacent list, that also includes the participating medical facilities, link to that study site's section on the Study Sites page in the website.
- Atlanta, GA: Emory University
- Aurora, CO: Barbara Davis Center for Diabetes - University of Colorado
- Baltimore, MD: Johns Hopkins
- Charleston, SC: Medical University of South Carolina
- Columbus, OH: Nationwide Children's Hospital
- Dallas, TX: Baylor, Scott & White Health
- Durham, NC: Duke University
- Houston, TX: Texas Children's Hospital - Baylor College of Medicine
- Iowa City, IA: University of Iowa
- Nashville, TN: Vanderbilt University Medical Center
- New Orleans, LA: Ochsner Health System
- Palo Alto, CA: Stanford Children's Hospital
- Philadelphia, PA: Children's Hospital of Philadelphia
- Pittsburgh, PA: University of Pittsburgh Medical Center
- Rochester, MN: Mayo Clinic
Researchers at Vanderbilt University Medical Center have received a grant from the National Institute of Diabetes and Digestive and Kidney Diseases, part of the National Institutes of Health, to study the relationship between various factors – such as COVID-19 infections, diabetes medications, diet and exercise – and diabetes. The study will partner with Harvard, Children’s Hospital of Philadelphia, Weil Cornell Medical Center, Stanford University, the Type 1 Diabetes Exchange, and the University of Pittsburgh Medical Center to oversee the study. In addition, the sites listed above will help with recruiting and following study participants.
The COVID-19 and Diabetes Assessment (CODA) Study will identify and recruit participants through the T1D Exchange and health systems that participate in PCORnet. The T1D Exchange is a nonprofit research network of diabetes centers, dedicated to improving outcomes for people with Type 1 Diabetes. PCORnet is a national research network funded by the Patient-Centered Outcomes Research Institute, which engages hundreds of health care sites across the country.
The Study will enroll about 1,000 patients. All participants must be age 11 or older, and been diagnosed with diabetes in the last six months.
CODA's goal is to gain a deeper understanding of what happens in early diabetes in order to guide future treatment interventions and public health approaches. CODA will be led by a team of scientists with significant experience in treating and understanding COVID-19, obesity and diabetes in children and adults.
Dr. Rothman, the Ingram Professor of Integrative and Population Health and professor of Internal Medicine, Pediatrics, and Health Policy at Vanderbilt, is also VUMC Senior Vice President for Population and Public Health, and director of the Vanderbilt Institute for Medicine and Public Health.
Co-principal investigators are:
- Alvin Powers, MD, the Joe C. Davis Professor of Biomedical Science, professor of Medicine and of Molecular Physiology and Biophysics, director of the Vanderbilt Diabetes Center and of the Vanderbilt Diabetes Research
- Jonathan Schildcrout, PhD, professor of Biostatistics and Anesthesiology at VUMC. Leading the Vanderbilt Biostatistics Data Coordinating Center.
- Jason Block, MD, MPH, associate professor of Population Health in the Harvard Pilgrim Health Care Institute.
Diabetes is an illness characterized by high levels of blood glucose, which increase the risk for heart and kidney disease, nerve and eye damage, and other serious complications. It results from the body's inability to make or respond to insulin, a hormone that promotes glucose uptake by the tissues.
Type 1 diabetes, which usually is diagnosed in children, results from destruction of the beta cells of the pancreas, which make insulin. Type 2 diabetes is the most common form of the disease. It usually develops later in life and occurs when body tissues do not respond (become resistant) to insulin.
CODA will explore:
- Whether participants diagnosed with COVID-19 who then developed Type 2 diabetes are more likely to have worse blood sugar control, increased inflammation, and increased insulin resistance than patients with Type 2 diabetes but without a recent COVID-19 diagnosis.
- Whether participants with a recent diagnoses of COVID-19 who then developed Type 1 diabetes are more likely to have worse blood sugar control, increased inflammation, and a more rapid reduction in the function of their beta cells than those without a recent COVID-19 diagnosis.
- Whether COVID-19 is associated with worse vascular function, increased inflammation, and an increased tendency to form blood clots within blood vessels in a subset of participants with diabetes.
- The role of genetic, social, and environmental factors on inflammation and metabolic function
- The impact of COVID-19 and its treatments on the development of diabetes and on diabetes-related outcomes over the course of time
- Individuals who agree to participate in the study will be surveyed by phone, online, or in person and will provide regular blood samples. Some participants will have glucose tolerance, biomarkers and vascular function testing. The study will also use longitudinal electronic health record data from participating sites and across PCORnet.
The research is supported by the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK), a branch of the U.S. National Institutes of Health (NIH). The CODA Study is funded by the NIDDK/NIH (Grant # 1U01DK137533).



